
A ketogenic diet may have done more than trim carbs in a small group of adults with type 2 diabetes. It was linked to better beta-cell function, the pancreas’s ability to make and release insulin, which matters because stressed beta cells make blood sugar control harder as diabetes advances.
The study randomized 51 adults with type 2 diabetes to either a ketogenic diet or a low-fat diet for 12 weeks. Participants were 55 years old on average, 76% were female, and 54% were African American. Both eating plans were designed to maintain weight, not drive major weight loss, yet both groups still lost a modest amount on average. That makes the signal more interesting: the keto group showed a larger drop in the share of proinsulin being secreted, a marker tied to beta-cell stress.
Researchers used a hyperglycemic clamp, one of the more demanding ways to test insulin secretion, to measure acute and maximal C-peptide responses and beta-cell function. The key result was not just a change in glucose numbers. Diet assignment significantly predicted a lower fasting proinsulin-to-C-peptide ratio and a lower 190-minute proinsulin-to-C-peptide ratio in the ketogenic group compared with the low-fat group. Changes in acute C-peptide response moved in the opposite direction of the ratio, reinforcing the idea that the pancreas may have been working more efficiently.
That distinction matters for readers curious about keto. Better beta-cell function does not mean diabetes was reversed. It means the cells that produce insulin appeared to be under less strain and able to respond better after three months. Glucose changes were similar across the two diets, so the study’s main message was not simple short-term blood sugar lowering. It pointed instead to a possible effect on pancreatic stress itself.

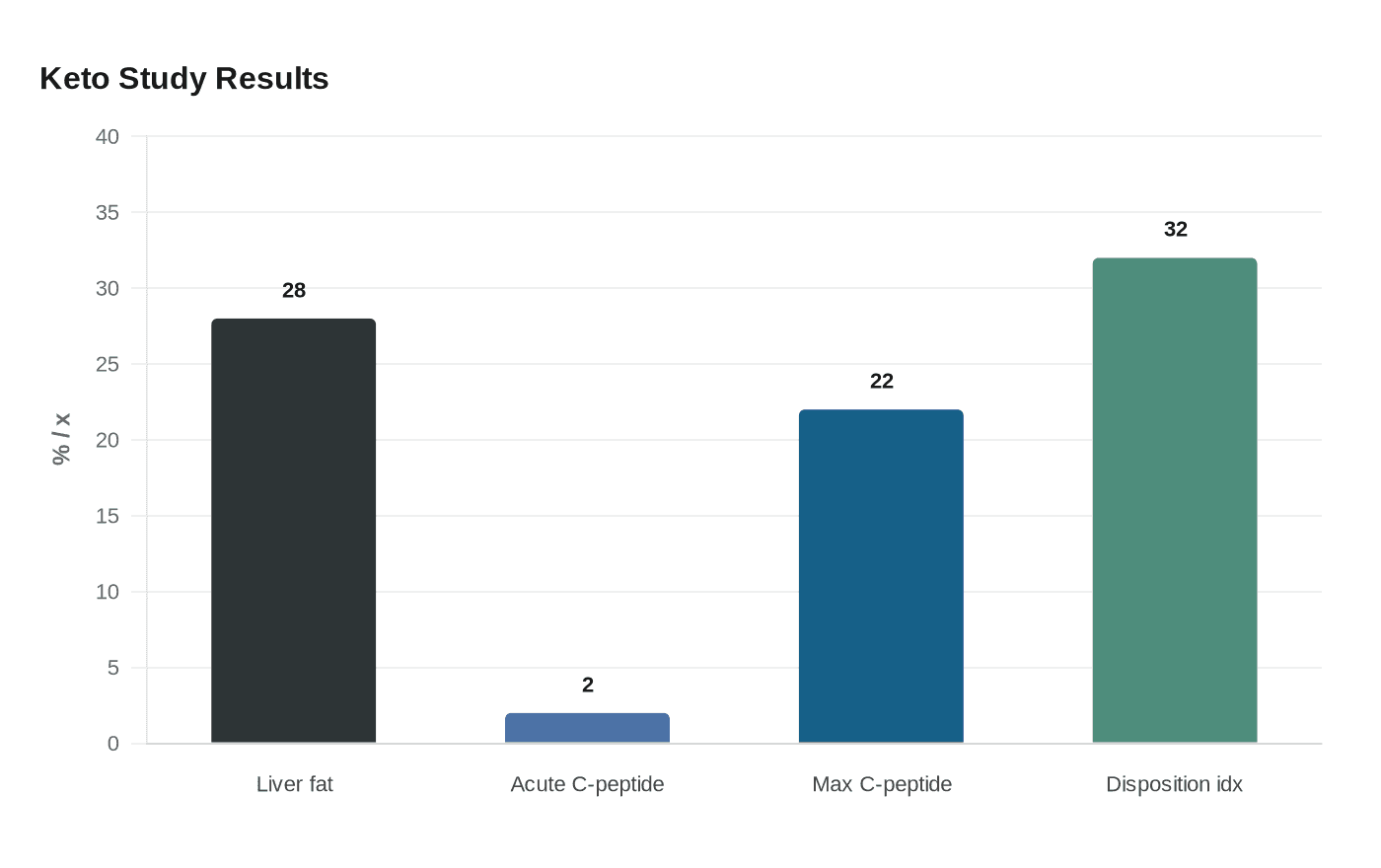
The finding fit a broader pattern from the same University of Alabama at Birmingham research group. A paper published January 20, 2026, reported that a eucaloric ketogenic diet in 57 adults with mild type 2 diabetes reduced liver fat by 28% and lowered de novo lipogenesis markers, alongside restored beta-cell function. A separate randomized trial in 57 adults with type 2 diabetes found that a carbohydrate-restricted diet produced a 2-fold greater acute C-peptide response, 22% greater maximal C-peptide response, and 32% greater disposition index than a higher-carbohydrate diet.
The new study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases, the Nutrition Obesity Research Center at the University of Alabama at Birmingham, the Diabetes Research Center at UAB, and the National Heart, Lung, and Blood Institute. It adds to a growing case that very low-carb eating may help some people with early type 2 diabetes, but it still stops well short of proving keto reverses the disease. The American Diabetes Association’s 2026 Standards of Care continue to push individualized, evidence-based nutrition rather than one fixed diet for everyone.
This article was produced by Prism’s automated news system from verified source data, official records, and press releases, then run through automated quality and moderation checks before publishing. The system is built and supervised by the people who set the standards it runs under. Read our full AI policy.
Know something we missed? Have a correction or additional information?
Submit a Tip

%3Amax_bytes(150000)%3Astrip_icc()%2F1036682-d776599ed42a484b88430e2a23025ed2.jpg&w=1920&q=75)